Helpline :
9807 55 6789
-
Call Us Now: 9807 55 6789Call Us Now: 9807 55 6789
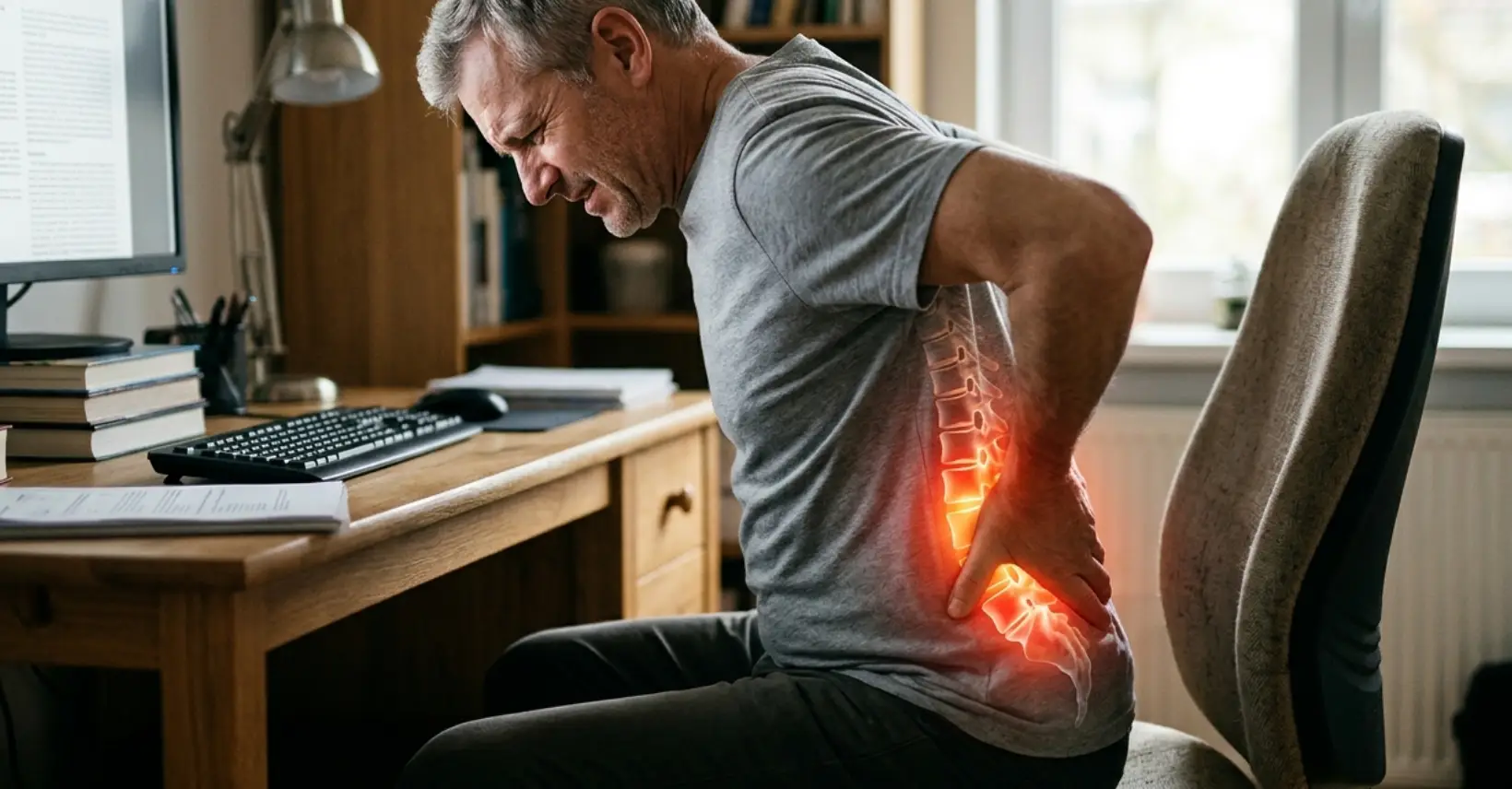
Low back pain whether from a slipped disc, spondylosis, sciatica or spondylolisthesis is one of the leading causes of disability worldwide. At IBAP Clinics, our UK-trained interventional pain specialist provides precise, non-surgical solutions targeted to the root cause of your pain.
Higher Specialist Training on the South East of England deanery rotation. Breadth of complex anaesthetic experience including regional, cardiac, and neuro-anaesthesia at University Teaching Hospitals.
Low back pain refers to pain arising between the lower rib margin and the buttocks, with or without radiation into the legs. It is classified as acute (less than 4 weeks), subacute (4–12 weeks), or chronic (lasting more than 12 weeks) and is the leading global cause of years lived with disability.
Think of the lumbar spine as the load-bearing arch of a bridge. Five vertebrae (L1–L5) stack upon each other, cushioned by intervertebral discs, stabilised by facet joints and ligaments, and traversed by a network of nerves. When any element of this system is damaged, degenerated or inflamed, pain results sometimes locally, sometimes radiating far from its source.
Crucially, the same underlying spinal pathology can present in different ways depending on which structure is affected as disc pain, nerve root pain, facet joint pain, or muscular pain. This is why accurate diagnosis before treatment is central to what we do at IBAP Clinics.

Understanding the anatomy explains why so many related conditions share the same origin.
The bony building blocks of the spine. Fractures, slippage (spondylolisthesis) or degeneration originate here.
Shock-absorbing cushions between each vertebra. Herniation or degeneration causes disc pain and nerve compression.
Small paired joints behind each disc. Arthritis of these joints (spondylosis) is among the most common causes of axial back pain.
Exit the spinal canal via foramina. Compression causes radiculopathy the shooting leg pain known as sciatica.
Dynamic stabilisers of the spine. Strain, spasm and trigger points account for a significant proportion of acute back pain.
Where the lumbar spine meets the pelvis. Responsible for 15–30% of chronic low back pain presentations.
Low back pain is rarely a diagnosis in itself — it is a symptom with many potential causes. The conditions below are all variants or progressions of the same spinal pathology continuum. Each has its own dedicated page with detailed information.
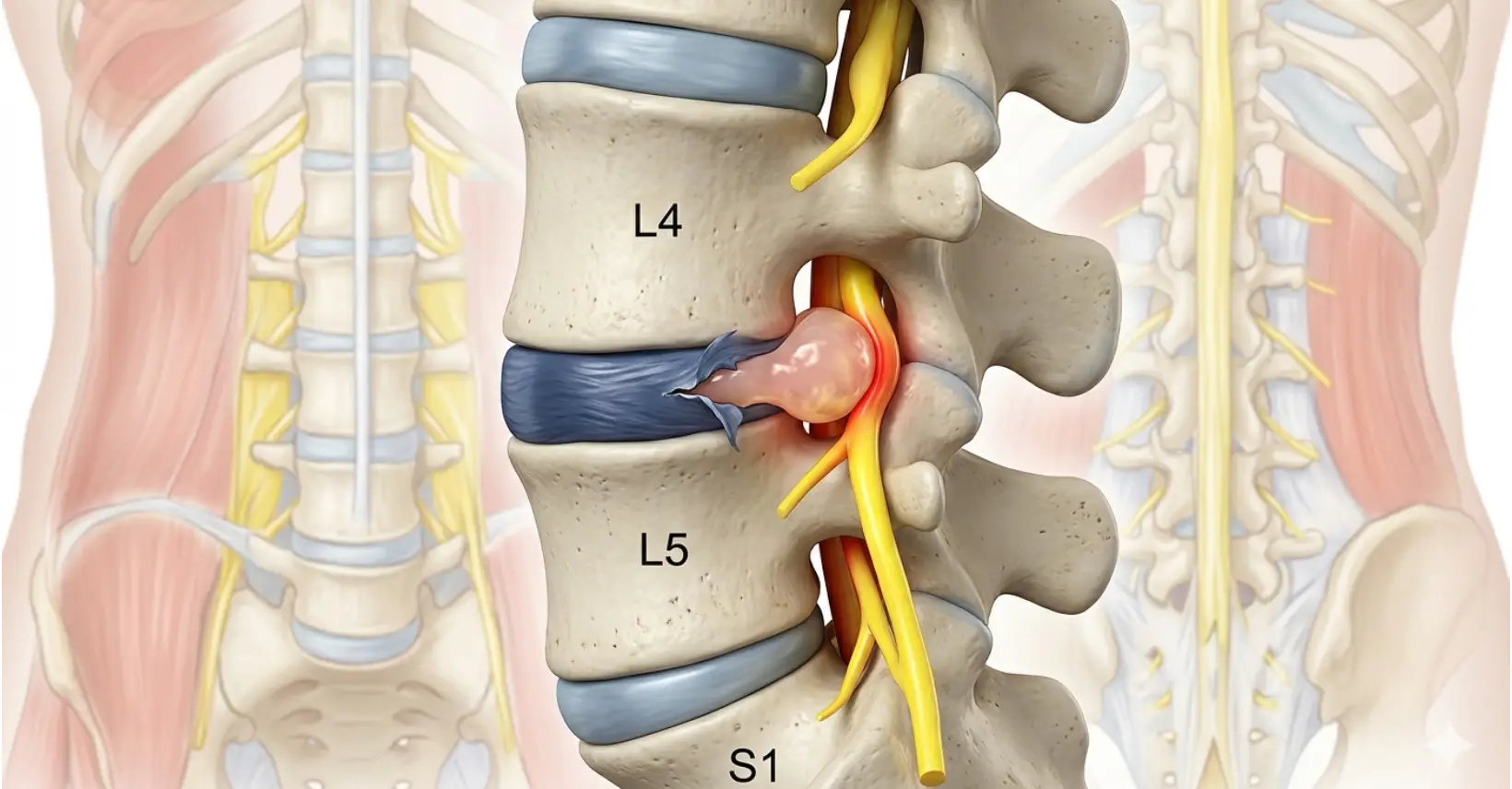
When the soft inner nucleus of a disc herniates through its outer ring, pressing on nearby nerve roots. Also called herniated disc, prolapsed disc or ruptured disc.
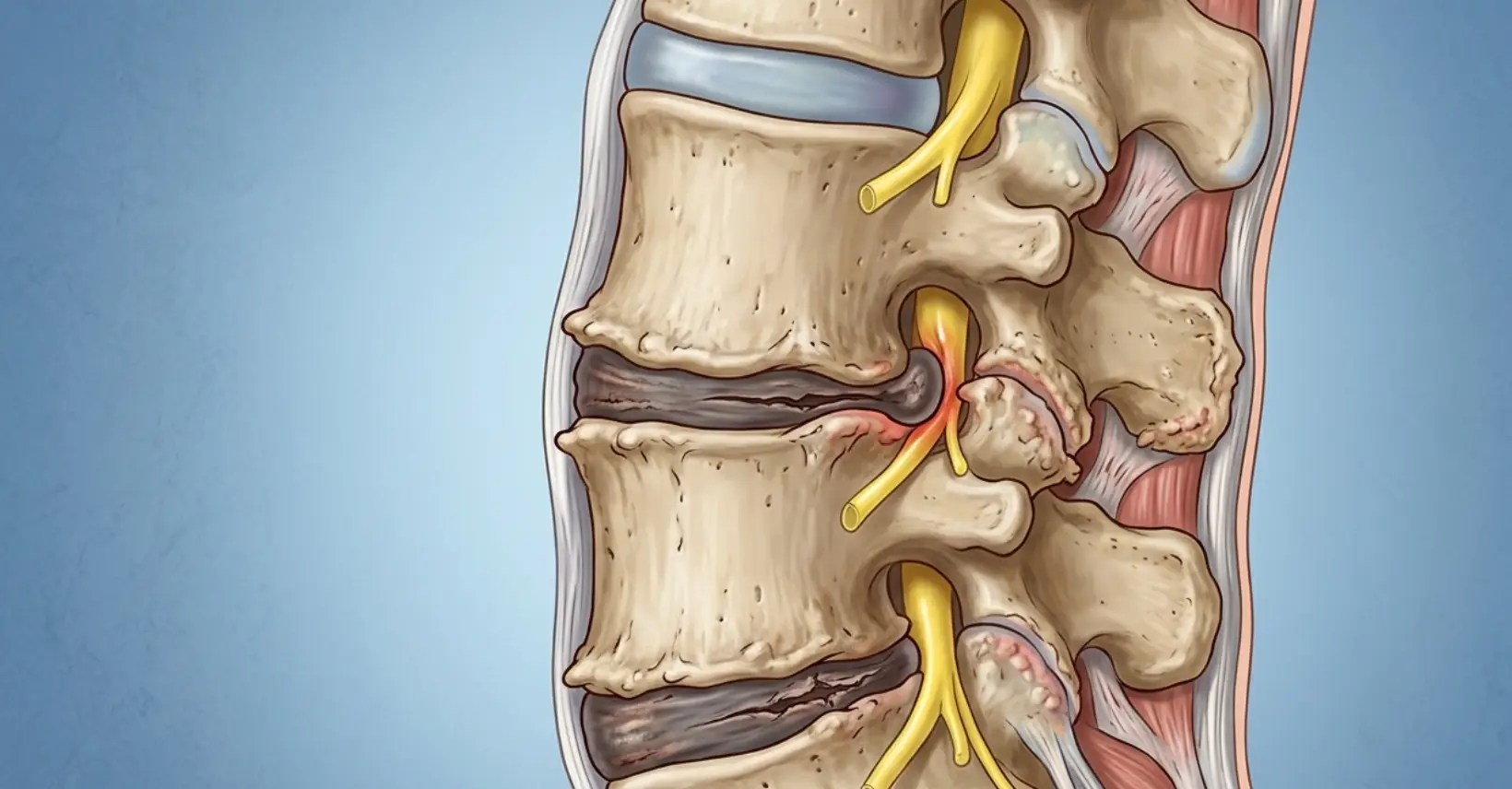
Age-related wear and tear of the discs, facet joints and vertebral end-plates. Disc degeneration occurs in over 80% of adults over the age of 50.
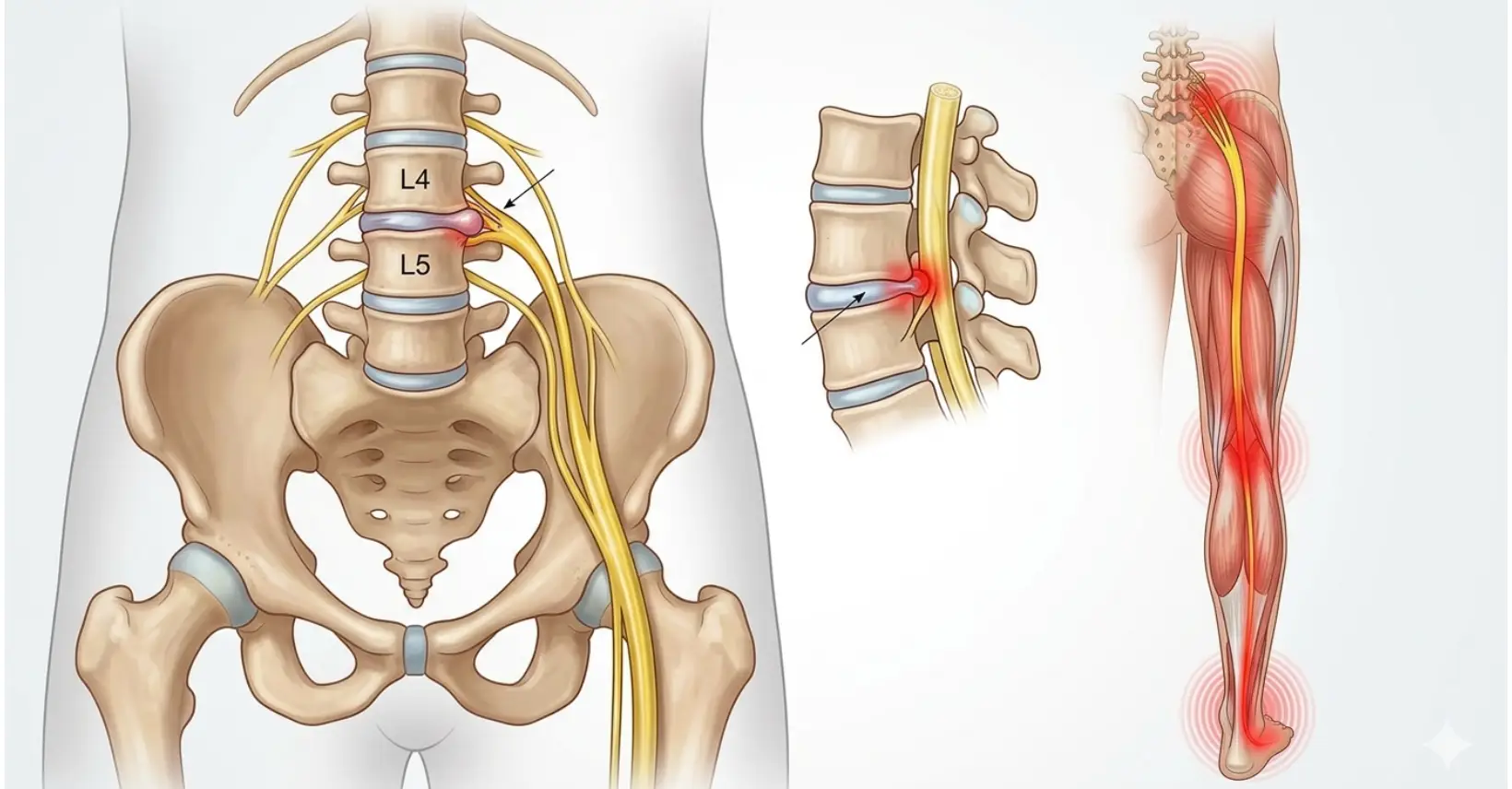
Compression or irritation of the sciatic nerve, causing pain, numbness or tingling to radiate from the lower back through the buttock and down the leg.
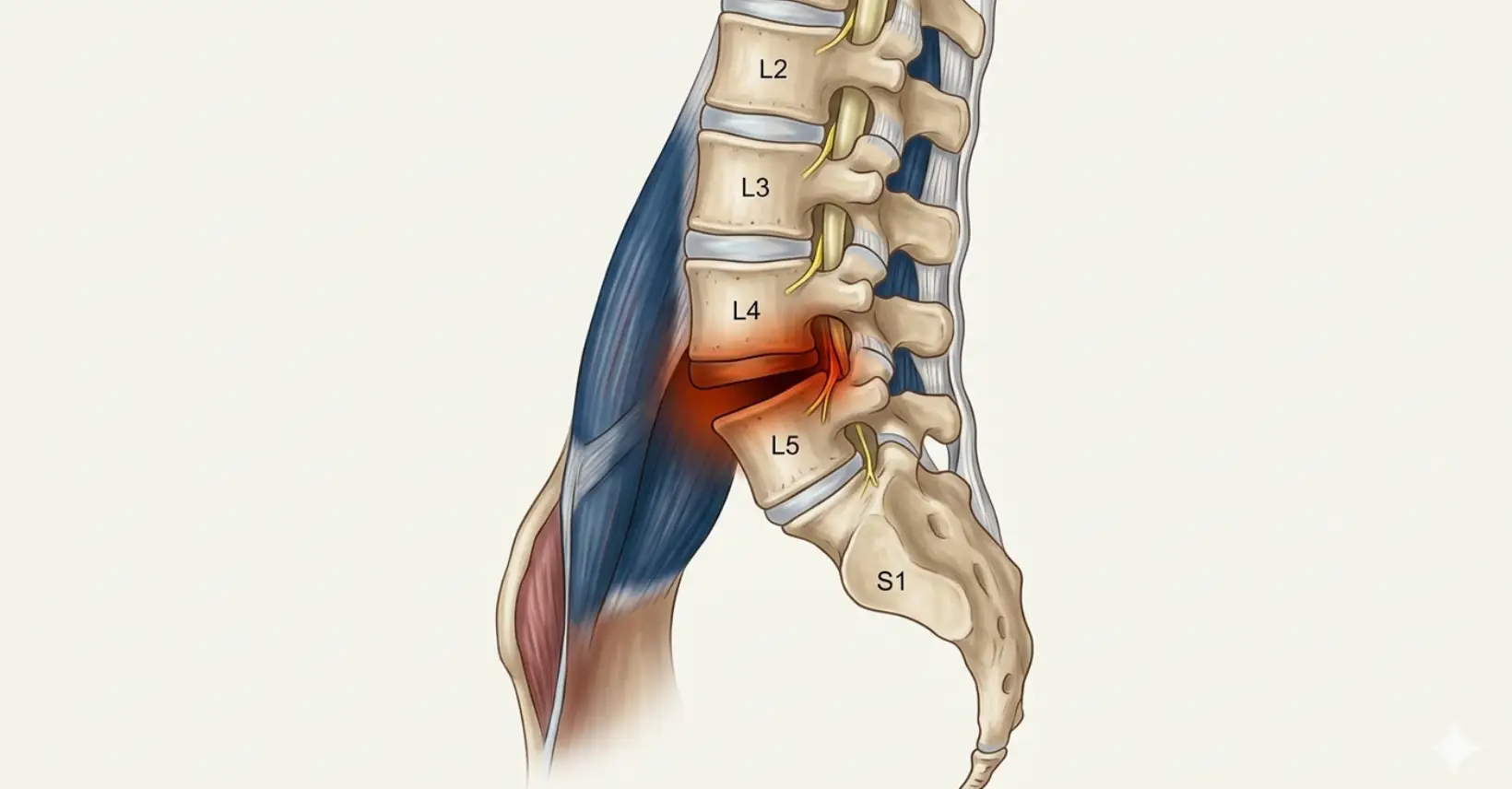
Forward slippage of one vertebra over another, most commonly at L4–L5 or L5–S1. Ranges from mild instability to significant nerve compression requiring intervention.
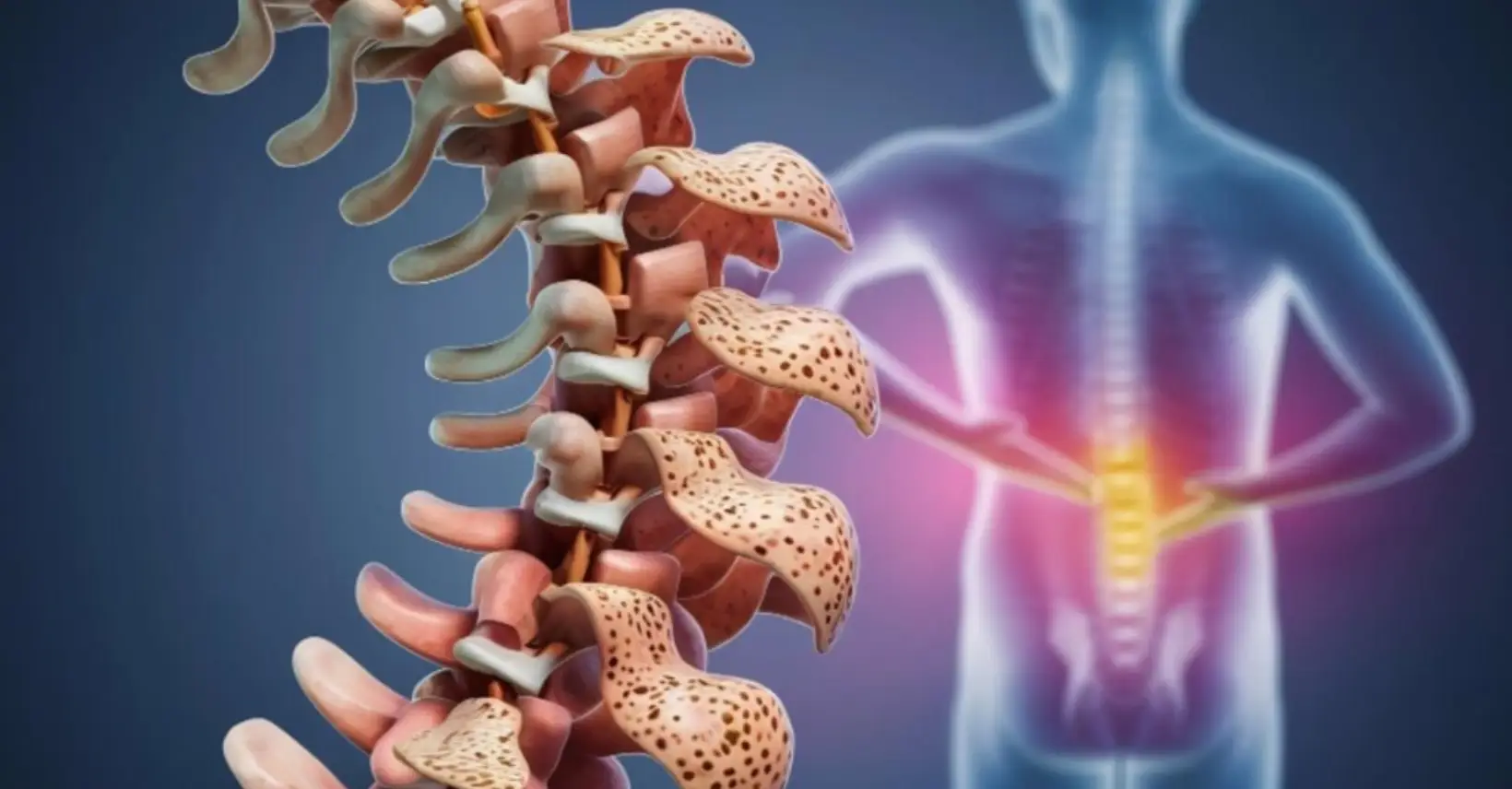
Inflammation of the vertebral joints — most notably Ankylosing Spondylitis (AS) and related spondyloarthropathies. Unlike mechanical back pain, spondylitis is immune-mediated and typically presents with early-morning stiffness lasting over 30 minutes, improving with activity rather than rest.
An older clinical term for non-specific low back pain. In modern pain medicine, lumbago is assessed to identify its structural cause rather than treated as a standalone diagnosis.
Low back pain presents differently depending on the underlying cause. The following are the most commonly reported symptoms that bring patients to IBAP Clinics.
The following symptoms alongside back pain require immediate evaluation and must not be ignored :

At IBAP Clinics, we believe in treating the cause, not just the symptom. Accurate diagnosis is the cornerstone of effective pain management. Our process mirrors the best of UK and international interventional pain practice.

A thorough consultation exploring the nature, onset, character, radiation and aggravating factors of your pain. We use validated pain assessment tools alongside a functional disability evaluation.

Assessment of spinal mobility, nerve tension signs (straight leg raise, femoral stretch test), muscle strength, reflexes and sensory function to localise the pain generator.

Before proceeding to static imaging, we assess how your spine moves and loads. Digital Spinal Analysis (DSA) is a computerised, posture-based functional assessment that measures spinal alignment, range of motion, load distribution, and postural deviations in real time. Think of it as an ECG for your spine whereas X-ray or MRI shows structure, DSA shows function. It identifies compensatory patterns, muscle imbalances and biomechanical stress points that static imaging cannot reveal, allowing us to understand not just what is painful, but why it became painful and how to correct it.

Imaging is interpreted within the clinical context. Degenerative changes are common in asymptomatic adults — imaging findings alone do not determine treatment. MRI is the gold standard for soft tissue, disc and nerve assessment.

Targeted diagnostic nerve blocks — such as medial branch blocks or selective nerve root blocks — can confirm the pain source with precision before proceeding to definitive treatment.

Based on all the above, a tailored treatment pathway is designed — ranging from targeted injections and nerve blocks to radiofrequency ablation, regenerative therapies or neuromodulation for complex cases.
Our treatment philosophy is precision over generalisation. We match the intervention to the diagnosis — guided by fluoroscopy or ultrasound — to maximise efficacy and minimise risk. All procedures are performed to UK interventional pain standards.

Targeted delivery of therapeutic agents to the precise pain source under fluoroscopic guidance
Fluoroscopy-guided delivery of corticosteroid into the epidural space to reduce nerve root inflammation. Available as interlaminar, transforaminal or caudal routes depending on the pain source. Evidence supports significant relief in disc herniation with radiculopathy.
Intra-articular steroid injections or nerve blocks targeting the medial branches that supply the facet joints. Used for diagnosis and treatment of spondylosis and facet-mediated axial low back pain.
Precise steroid delivery alongside a specific nerve root — the most targeted epidural technique. Particularly effective for single-level disc herniation causing sciatica, and recommended before considering surgery.
The sacroiliac joint accounts for 15–30% of chronic low back pain. Targeted intra-articular injections and radiofrequency denervation of the SI joint are highly effective when the SI joint is confirmed as the pain source.

Energy-based denervation to interrupt pain signals — from conventional heat to cold and pulsed approaches
Thermal denervation of medial branch nerves using continuous radiofrequency energy (80–90°C). The gold standard for confirmed facet joint pain — providing 12–24 months of sustained relief. A day-care, minimally invasive procedure with a robust evidence base.
A refinement of conventional RFA that circulates cooled water through the probe tip, creating a larger, more consistent lesion at a controlled temperature. Particularly advantageous for the sacroiliac joint and targets where precise anatomy makes standard RFA less reliable. Produces a broader ablation zone without increased tissue charring.
Rather than heat, cryoablation uses extreme cold (–70°C) to disrupt nerve conduction causing Wallerian degeneration without destroying the nerve sheath. This allows nerve regeneration over time, making it reversible in nature. Particularly useful in post-surgical pain, peripheral nerve entrapments and patients who prefer a non-heat approach.
Pulsed RF delivers radiofrequency energy in short bursts (milliseconds on, seconds off), keeping tissue temperature below 42°C. Unlike thermal RFA, it modulates rather than destroys nerve tissue — making it suitable for sensory nerve roots, dorsal root ganglia and peripheral nerves where thermal ablation carries risk of neuritis or deafferentation pain.

Minimally invasive treatments delivered directly into the disc — targeting the source of discogenic pain
A mixture of oxygen and ozone gas is injected directly into the nucleus pulposus of the herniated disc. Ozone oxidises the proteoglycans responsible for water retention, causing the disc to shrink and decompress the nerve root. It additionally exerts powerful anti-inflammatory and analgesic effects. A minimally invasive, radiation-free alternative to surgical discectomy widely practised in Europe and increasingly adopted in India.
Two cooled radiofrequency probes are placed within the disc and positioned on either side of the posterior annulus. Bipolar RF energy is delivered between them, heating and denaturing the pain-generating nerve fibres in the annular wall. Unlike older thermal techniques (IDET), biacuplasty produces a controlled, even lesion with minimal risk to the nucleus specifically designed for internally disrupted, painful discs (discogenic axial pain).
A fine laser fibre is introduced into the disc via a needle under fluoroscopic guidance. Laser energy vaporises a small volume of nucleus pulposus, reducing intradiscal pressure and allowing the herniation to retract away from the nerve root. Percutaneous Laser Disc Decompression (PLDD) is effective for contained disc herniations where decompression of the nucleus is the primary therapeutic goal without any incision or general anaesthesia.

Harnessing the body's own biology to repair, regenerate and reduce inflammation — moving beyond symptom suppression
A concentrated preparation of growth factors derived from your own blood including PDGF, TGF-β and VEGF injected into degenerated discs, facet joints or the epidural space. PRP promotes tissue repair, modulates inflammation and stimulates disc cell proliferation. An effective non-steroid regenerative option for discogenic pain, early spondylosis and post-procedural recovery enhancement.
Bone Marrow Aspirate Concentrate (BMAC) is harvested from the patient’s own iliac crest and concentrated to yield a rich mixture of mesenchymal stem cells, haematopoietic progenitors, growth factors and cytokines. At IBAP Clinics, BMAC is deployed in two key ways: intradiscal injection — to regenerate degenerated disc tissue, restore disc height and reduce discogenic pain; and epidural delivery — to promote nerve root healing, reduce perineural inflammation and facilitate neuroregenerative repair in chronic radiculopathy. BMAC represents the cutting edge of autologous regenerative spine medicine.

Structural restoration of fractured or collapsed vertebrae — providing immediate pain relief and spinal stability
A minimally invasive fluoroscopy-guided procedure in which bone cement (PMMA) is injected under pressure directly into a fractured or osteoporotic vertebral body. Vertebroplasty stabilises the fracture, prevents further collapse and provides rapid pain relief — often within 24–48 hours. Indicated for painful vertebral compression fractures due to osteoporosis, cancer-related vertebral involvement or trauma.
A refinement of vertebroplasty in which an inflatable balloon tamp is first introduced into the fractured vertebra and expanded to restore vertebral height and create a cavity — before cement is injected at low pressure. Kyphoplasty not only stabilises the fracture and relieves pain, but also corrects kyphotic deformity, improving posture and reducing the risk of adjacent level fractures. The gold standard for vertebral augmentation in painful osteoporotic compression fractures.

For complex, refractory or chronic pain where all other options have been exhausted
For patients with chronic refractory low back pain or failed back surgery syndrome, neuromodulation via spinal cord stimulation can achieve sustained pain relief where all other treatments have failed. Dr Vijay holds a dedicated Fellowship in Neuromodulation and Advanced Pain (London).
For severe, refractory spinal pain, an intrathecal drug delivery system delivers medication directly into the spinal fluid at a fraction of the oral dose — minimising systemic side effects while maximising pain control.
IBAP Clinics was founded on a single conviction: every patient with chronic pain deserves access to world-class, evidence-based interventional pain management without travelling abroad.
Dual Fellowship from the Royal College of Anaesthetists (London) — among the highest pain medicine qualifications in the world
Advanced Pain Training (Cambridge) and Fellowship in Neuromodulation & Advanced Pain (London)
All spinal interventions performed under live fluoroscopy — the same standard as leading UK pain centres
We exhaust every evidence-based non-surgical option before any surgical referral is considered
PRP and biologics available alongside traditional interventional therapies for a complete pain management portfolio
Banjara Hills (Main) and Madeenaguda (Branch) — serving patients across greater Hyderabad
These questions are among the most commonly searched by patients with low back pain. Answers are provided by Dr Vijay Bhaskar, Interventional Pain Specialist, IBAP Clinics.
The most common causes of low back pain are mechanical in nature — meaning related to the spine’s structures rather than systemic disease. These include degenerative disc disease (wear and tear of the intervertebral discs), facet joint arthritis (spondylosis), herniated or slipped disc (pressing on nearby nerves), muscle or ligament strain, and sacroiliac joint dysfunction. Over 90% of low back pain presentations are non-specific mechanical pain that can be managed without surgery when properly diagnosed and treated.
Yes — the vast majority of low back pain, including slipped disc, spondylosis, sciatica and spondylolisthesis, can be successfully managed without surgery. Interventional pain treatments such as epidural steroid injections, radiofrequency ablation, facet joint blocks, transforaminal nerve root blocks and regenerative therapies like PRP offer targeted, evidence-based relief. Surgery is reserved for a small minority of cases with severe structural instability, cauda equina syndrome, or those who have not responded to conservative and interventional management.
Low back pain is pain localised to the lumbar region of the spine. Sciatica is a specific subtype where the sciatic nerve — the longest nerve in the body — is compressed or irritated, causing pain to radiate from the lower back through the buttock and down the leg, sometimes reaching the foot. Sciatica is most often caused by a slipped disc or bone spur pressing on a nerve root at L4, L5 or S1. It is a symptom, not a diagnosis, and identifying the exact nerve root and cause is essential for targeted treatment.
Yes — these terms all describe the same condition. A slipped disc, herniated disc, prolapsed disc and ruptured disc all refer to when the soft gel-like nucleus (nucleus pulposus) of an intervertebral disc pushes through a tear or weakness in the tougher outer ring (annulus fibrosus). This material can press on adjacent nerve roots, causing local back pain, sciatica, numbness or muscle weakness. The term “slipped disc” is a slight misnomer — the disc does not actually slip out of place; rather, its contents herniate.
You should seek specialist care if your low back pain: (1) lasts longer than 6 weeks without improvement; (2) is getting progressively worse; (3) is accompanied by leg numbness, tingling or weakness; (4) is interfering with sleep or daily activities; or (5) is not responding to physiotherapy and over-the-counter pain medications. Additionally, any of the red flag symptoms listed on this page (such as bladder/bowel dysfunction or bilateral leg weakness) require urgent same-day assessment.
At IBAP Clinics, Hyderabad, we offer a full spectrum of evidence-based interventional treatments including epidural steroid injections (interlaminar, transforaminal and caudal), medial branch blocks, facet joint injections, radiofrequency ablation, sacroiliac joint interventions, PRP regenerative therapy, intradiscal procedures and — for refractory complex pain — spinal cord stimulation and intrathecal drug delivery systems. All procedures are performed under fluoroscopic guidance to the same standards practised in leading UK pain centres.
Spondylolisthesis occurs when one vertebra slips forward over the vertebra below it — most commonly at L4–L5 or L5–S1. It is graded I–IV based on severity. Grade I and II spondylolisthesis (less than 50% slip) are typically managed non-surgically with targeted physiotherapy, epidural injections and radiofrequency denervation to control pain and stabilise the affected segment. Grade III–IV or rapidly progressive cases may require surgical stabilisation. At IBAP Clinics, we thoroughly assess each case and will only refer for surgery when non-surgical options have been appropriately trialled.
2nd Floor, 284/A, Road No. 12, above IDFC First Bank, near Omega hospitals, MLA Colony, Banjara Hills, Hyderabad, Telangana 500034.
4th Floor, Plot no. 200, beside South India Shopping Mall, opp. Fortune Heights, Madeenaguda, Hyderabad, Telangana 500049

Indo-British Advanced Pain Clinic © 2026. All Rights Reserved. Designed & Developed By Adroit
WhatsApp us