Helpline :
9807 55 6789
-
Call Us Now: 9807 55 6789Call Us Now: 9807 55 6789
A comprehensive guide to cervical pain — from everyday tech neck and road-accident whiplash to pinched nerves and rare serious causes — authored by Hyderabad’s leading interventional pain specialist.

This is the central hub. Each spoke below links to a detailed condition-specific page.
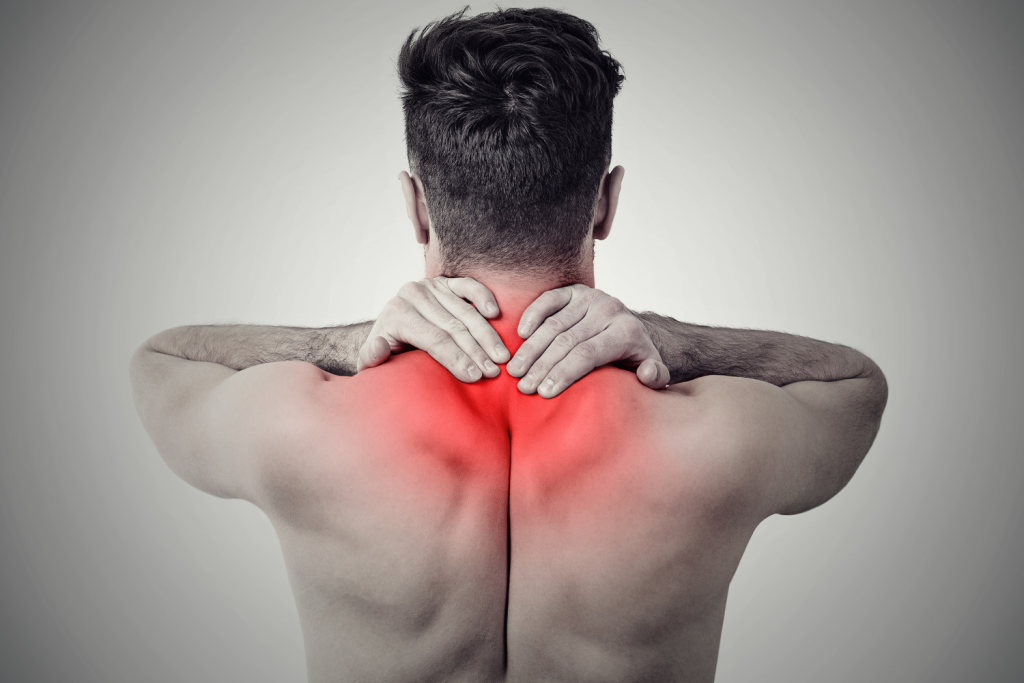
Postural cervical strain from screens
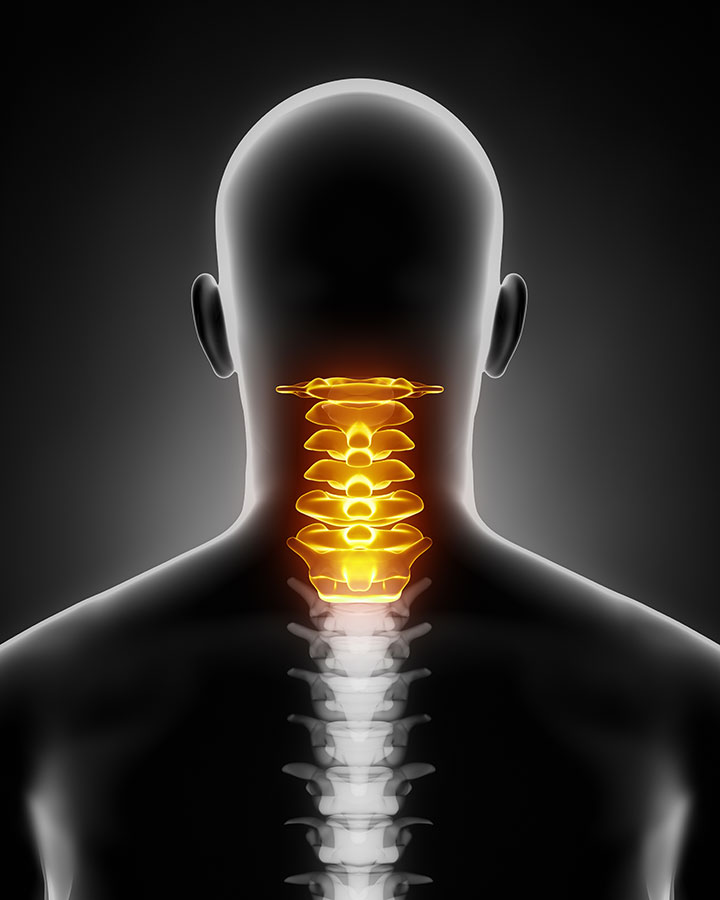
Slipped disc, pinched nerves
Arthritis & age-related wear
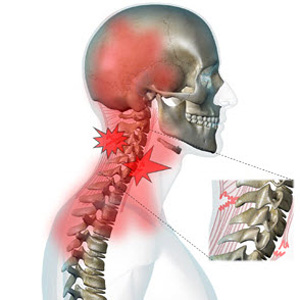
Road accidents, trauma,Whiplash
Neck-sourced head pain
Blocks, RF, SCS & more

Cancer, infection, inflammatory
The cervical spine comprises seven vertebrae (C1–C7) stacked like a flexible tower of rings. Between each ring sits a disc — a shock-absorbing cushion with a tough outer shell (annulus fibrosus) and a gel-like core (nucleus pulposus). Running through the middle of this tower is your spinal cord, and branching off at each level are the nerve roots that travel into your arms, shoulders, and even influence your hands and fingers.
Think of it this way
The cervical spine is like a garden hosepipe supported by seven cotton reels. The hose carries electrical signals (nerve impulses); the reels are the vertebrae; and the rubber washers between them are the discs. Unlike the low back, which has the pelvis to anchor it, or the thoracic spine, braced by the ribcage, the neck stands alone — balancing a bowling-ball-weight head (5–6 kg) on seven relatively small bones, all day, every day. Any compression, poor posture, or injury that deforms these components can irritate or pinch the hose — and that is neck pain with arm symptoms (radiculopathy).
Unlike the low back or knee, the neck also hosts critical blood vessels (vertebral arteries), lymph nodes, the thyroid gland, and the oesophagus — meaning neck pain sometimes signals conditions far from the spine, making accurate diagnosis essential.
Neck pain rarely has a single cause. More often, it results from a combination of structural vulnerability, lifestyle habits, and precipitating events. Here in Hyderabad, several uniquely local factors stack the odds against a healthy cervical spine.
📱
The single biggest driver of neck pain in urban India. Scrolling through social media, attending back-to-back video calls on laptops, or hunching over IT workstations for 10–14 hours daily places the cervical spine under enormous flexion stress. For every inch the head tilts forward, the effective load on the neck doubles. At a 45° forward tilt — typical smartphone posture — the neck muscles experience the equivalent of carrying a 22 kg weight. Hyderabad’s IT corridor and software parks make this an occupational epidemic.
These symptoms in the context of neck pain require urgent medical assessment. Do not wait.
One of the most under-recognised and mis-treated causes of chronic headache. Cervicogenic headache originates from the upper cervical spine (C1–C3 joints and the greater occipital nerve) and is felt as a unilateral, non-throbbing ache starting at the back of the head and radiating to the forehead, temple, or eye. It is frequently misdiagnosed as migraine or tension headache. Key clue: the headache is provoked or worsened by neck movement or pressure on the upper cervical joints. Treatment targets the cervical source — nerve blocks, medial branch blocks, or radiofrequency ablation — rather than conventional migraine therapy.
When a disc herniation or osteophyte compresses a cervical nerve root, pain radiates in a specific pattern down the arm — like a “shock” or “electric” sensation following the nerve’s territory. C6 compression causes thumb and index finger symptoms; C7 affects the middle finger; C8 involves the ring and little fingers. This is distinct from peripheral nerve entrapment (see differential diagnoses) and confirms that the pain source is in the neck, not the arm or wrist.
A serious consequence of cervical spinal cord compression, causing progressive hand clumsiness, difficulty with fine motor tasks (buttoning a shirt, writing), unsteady gait, and bladder urgency. Unlike radiculopathy, myelopathy is a bilateral, progressive condition that represents true spinal cord injury. It is an important surgical consideration. Any patient with bilateral arm symptoms and gait disturbance must be assessed urgently.
A common pain condition involving trigger points — hyper-irritable, taut bands within neck and shoulder muscles (commonly the trapezius, SCM, and suboccipital muscles). These trigger points can refer pain to the head, arm, and chest in predictable patterns, mimicking cardiac or disc-related pain. Stress, poor posture, and overuse are the key drivers. Treatment involves trigger point injections, dry needling, physiotherapy, and addressing the underlying postural or psychological cause.
Compression of the brachial plexus and subclavian vessels as they exit between the collarbone and first rib — often related to cervical postural abnormalities, a cervical rib, or muscle hypertrophy. Produces arm pain, tingling, and occasionally colour changes in the hand. Can coexist with cervical disc disease, making accurate diagnosis critical.
Neck and shoulder pain frequently coexist, and the two often perpetuate each other. Cervical radiculopathy can cause shoulder weakness mimicking a rotator cuff tear; conversely, shoulder pathology can cause referred pain up into the neck. Distinguishing these requires careful clinical testing and targeted diagnostic injections.
Several conditions can masquerade as — or coexist with — cervical spine disease. Accurate diagnosis requires excluding these before committing to a cervical treatment pathway.
| Condition | Key Distinguishing Features | Why It Matters |
|---|---|---|
|
Myocardial Infarction (Heart Attack) Emergency |
Jaw pain, left arm pain, chest tightness, sweating, shortness of breath; pain does not change with neck movement | Life-threatening; misdiagnosis as neck pain is fatal |
|
Carpal Tunnel Syndrome (CTS) |
Tingling in thumb, index, and middle fingers; worse at night; Phalen's test positive; no neck movement triggers | Often coexists with C6 radiculopathy “double crush”; treating only the neck or only the wrist may fail |
|
Complex Regional Pain Syndrome (CRPS) |
Disproportionate, burning arm pain; skin colour/temperature changes; swelling; often post-trauma or post-surgery | Requires a specific, distinct treatment protocol; dramatically different from disc disease management |
|
Lateral Epicondylitis (Tennis Elbow) |
Localised elbow pain, tender over lateral epicondyle; provoked by wrist extension/gripping; no neck component | Can be confused with C6/C7 radiculopathy; coexists in manual workers and IT professionals |
|
Thoracic Outlet Syndrome |
Vascular limb pallor/cyanosis or neurogenic C8/T1 pattern weakness features; provoked by overhead arm positions | May mimic lower cervical disc disease; requires vascular and neurological assessment |
|
Shoulder Pathology (Frozen Shoulder / Rotator Cuff) |
Pain and restriction in shoulder rotation; Neer's/Hawkins' impingement positive; MRI shoulder, not spine, is diagnostic | Coexists with cervical disease; treating only one may leave the other untreated |
|
Vertebral Artery Dissection Emergency |
Sudden neck pain with new headache, dizziness, visual disturbance, facial numbness; often follows chiropractic manipulation or minor trauma | Stroke risk; requires emergency vascular imaging CT angiography |
|
Polymyalgia Rheumatica / Inflammatory Arthritis |
Morning stiffness >45 minutes; bilateral shoulder and hip girdle pain; markedly elevated ESR and CRP; age >60 | Responds to corticosteroids, not spinal interventions; untreated can cause giant cell arteritis and blindness |
The GPS Analogy
Think of differential diagnosis as entering the correct destination into a GPS before starting your journey. If you enter the wrong starting point — treating carpal tunnel syndrome as a cervical disc problem — you will never arrive at relief, no matter how skilled the driver or how advanced the procedure. Getting the diagnosis right is not a formality; it is the single most important step in the entire treatment journey.
At IBAP Clinics, we do not treat scans — we treat patients. A precise diagnosis requires listening carefully, examining thoroughly, and investigating intelligently. Our structured approach ensures no pain generator is missed and no unnecessary procedure is performed.
Detailed Clinical History
Pain character, onset, duration, radiation pattern, aggravating/relieving factors, occupational history, trauma history, red flag screening, psychosocial factors
Neurological & Physical Examination
Dermatome/myotome testing, reflexes, Spurling’s test, Lhermitte’s sign, upper motor neurone signs, cervical range of motion, provocative shoulder testing
MRI Cervical Spine
Gold standard for visualising disc herniations, cord compression, myelopathy, and soft tissue pathology. Dynamic flexion-extension MRI in selected cases
X-Ray & CT Scan
X-rays (AP, lateral, oblique, flexion-extension) assess alignment, instability, and osteophytes. CT provides excellent bony detail for foraminal stenosis, fractures, and surgical planning
Nerve Conduction Studies / EMG
Differentiates radiculopathy (nerve root) from peripheral neuropathy or entrapment (carpal tunnel, cubital tunnel). Essential in the double-crush scenario. Quantifies neurological damage
Blood Tests
ESR, CRP, RF, anti-CCP, ANA, CBC — to exclude inflammatory, infective, and haematological causes. HbA1c for diabetic neuropathy. PSA/tumour markers if malignancy suspected
Diagnostic Spinal Analgesia (DSA)
Precision diagnostic nerve blocks — medial branch blocks, selective nerve root blocks, or discography — used to confirm the exact pain generator before definitive interventional treatment
IBAP Principle: We believe in “diagnose before you treat.” A diagnostic nerve block that correctly identifies the pain source converts a non-responder into a responder and prevents unnecessary procedures at the wrong level. This is the standard of care in UK Pain Medicine and is practised rigorously at IBAP Clinics.
Before any interventional procedure, well-directed conservative treatment forms the foundation of neck pain management. In many cases of acute and sub-acute neck pain, this is sufficient.
Structured cervical stabilisation exercises, postural retraining, and manual therapy (mobilisation techniques) are the cornerstone of conservative management. Specific programmes address deep cervical flexor weakness — a universal finding in tech neck and chronic cervical pain.
When conservative measures provide insufficient relief, or when the cause is structural (disc, nerve, facet joint), targeted interventional procedures offer precise, effective, and minimally invasive treatment. At IBAP Clinics, all procedures are performed under image guidance (fluoroscopy or ultrasound) for accuracy and safety.
A corticosteroid delivered into the epidural space reduces perineural inflammation around compressed nerve roots. Effective for radiculopathy from disc herniation or foraminal stenosis. Performed under fluoroscopic guidance. Carries a higher risk profile than lumbar epidurals given the proximity to the spinal cord; performed by experienced interventionalists only.
A more targeted injection directly at the affected nerve root, delivering steroid precisely where it is needed. Particularly valuable when surgery is being considered — a positive SNRB at a specific level (e.g., C6) confirms that level as the pain generator and guides the surgeon’s approach. Carries a slightly higher risk than epidural injection and is performed with strict image guidance and contrast confirmation. At IBAP Clinics, SNRBs form a critical part of surgical pathway planning.
When facet joints (the small joints at the back of each vertebra) are the source of pain — typically causing axial neck pain and occipital headache — a corticosteroid injection into the joint or around the medial branch nerve provides targeted relief. Diagnosis is confirmed by a positive medial branch block.
When medial branch blocks confirm facet joint origin, radiofrequency ablation uses precisely applied heat to interrupt pain signals from the joint. Provides durable relief — typically 12–24 months — and can be repeated. The “gold standard” for facet-mediated cervical pain and cervicogenic headache.
For disc-generated neck pain (discogenic pain) where the disc itself is the pain source, these minimally invasive techniques address the problem at its root.
Medical-grade ozone gas is injected into the disc, shrinking the nucleus pulposus through oxidation and reducing the disc’s chemical pain-causing potential. A safe, well-tolerated procedure with growing evidence, particularly for contained herniations.
A minimally invasive procedure that uses radiofrequency energy delivered through two electrodes placed bilaterally within the disc to ablate the nociceptors in the annulus fibrosus — the pain-sensing nerve fibres in the disc’s outer layer. Particularly effective for discogenic pain.
A laser fibre is introduced into the disc via a fine needle under image guidance. Laser energy vaporises a small volume of the nucleus pulposus, reducing intradiscal pressure and the degree of herniation — achieving decompression of the nerve root without open surgery.
patients with failed conservative treatment or post-surgical pain, epidural adhesions and fibrosis can tether nerve roots. Adhesiolysis uses a specialised catheter to mechanically and chemically dissolve these adhesions and deliver targeted steroid and local anaesthetic directly to the affected nerve root.
Regenerative and neuromodulatory approaches for chronic cervical pain. Nanofat — a refined form of autologous adipose-derived stromal cells — delivers growth factors and anti-inflammatory signals to damaged cervical structures. These are emerging therapies offered within clinical frameworks at IBAP Clinics.
For severe, refractory cervical radiculopathy or post-surgical arm pain, a spinal cord stimulator delivers mild electrical pulses to the dorsal columns of the spinal cord, modulating pain signals before they reach the brain. A reversible, adjustable, evidence-based therapy for carefully selected patients. Dr Vijay Bhaskar holds a Fellowship in Neuromodulation from London and offers the full spectrum of SCS options.
In severe cancer pain or refractory benign pain, a programmable pump delivers opioid or non-opioid medication directly into the cerebrospinal fluid at a fraction of systemic doses — maximising efficacy and minimising side effects.
Surgery for neck pain is a significant decision. At IBAP Clinics, we follow a conservative-first philosophy informed by UK Pain Medicine training, evidence-based guidelines, and the principle that the risks of any intervention must be clearly outweighed by the expected benefit.
The Bridge Analogy
Think of surgery as replacing a section of a damaged bridge. If the bridge is weakened but functional — carrying traffic with some difficulty — targeted repairs (interventional procedures, physiotherapy) are far less disruptive than a full replacement. Surgery should be reserved for when the bridge is structurally failing and at risk of collapse, not merely because it has some cracks.
IBAP Practice:
When surgery is being planned, a positive Selective Nerve Root Block (SNRB) at the proposed surgical level provides critical confirmatory evidence. This ensures the surgeon operates at the correct level — an important safeguard in multilevel cervical disease. IBAP Clinics works collaboratively with neurosurgeons and spine surgeons to provide pre-operative diagnostic support where appropriate.
These questions are structured to appear in AI answer engines (Google SGE, Perplexity, ChatGPT) and voice search results. Each answer reflects the clinical practice of IBAP Clinics.
The most common cause of neck pain in Hyderabad is prolonged use of smartphones, laptops, and working at poorly set-up computer desks — collectively known as “tech neck” or cervical postural syndrome. Long hours of IT work, traffic driving, navigating Hyderabad’s potholes, and stress-related muscle tension are also major contributors. Hyderabad’s booming IT sector has made this an occupational epidemic, with many patients spending 10–14 hours daily in flexed cervical postures.
Seek emergency care if your neck pain is accompanied by: a sudden severe “thunderclap” headache (worst of your life), fever and neck stiffness (possible meningitis), weakness or numbness in both arms or legs, loss of bladder or bowel control, pain radiating to the jaw or left arm (possible heart attack), or neck pain following a road accident with any neurological change. These are red flags that require emergency evaluation — call 108 or go immediately to the nearest emergency department.
Yes — the vast majority of neck pain, including cervical disc herniations, spondylosis, and pinched nerves, can be successfully managed without surgery. Interventional pain procedures such as cervical epidural injections, selective nerve root blocks, radiofrequency ablation of facet joints, and intradiscal procedures like ozone disc nucleolysis or laser disc decompression offer effective, targeted, and minimally invasive relief. At IBAP Clinics, surgery is considered only when conservative and interventional measures have been exhausted, or when there is a clear threat to spinal cord function.
A cervicogenic headache originates from structures in the upper cervical spine — particularly the C1–C3 joints and the greater occipital nerve — and is felt as pain starting at the back of the head, radiating to the forehead, temple, or behind the eye. It is commonly misdiagnosed as migraine. Key distinguishing features include: unilateral headache provoked by neck movement, stiffness of the neck alongside the headache, and tenderness over the upper cervical joints. Effective treatment targets the cervical source using nerve blocks or radiofrequency procedures at IBAP Clinics.
IBAP Clinics offers the full spectrum of interventional pain procedures for neck pain: cervical epidural steroid injections, selective nerve root blocks (SNRB), cervical facet joint injections, medial branch radiofrequency ablation, ozone disc nucleolysis, biaculoplasty, percutaneous laser disc decompression (PLDD), epidurolysis, MAC and Nanofat regenerative procedures, and for severe refractory cases, spinal cord stimulation and intrathecal drug delivery systems. All procedures are performed under image guidance by Dr Vijay Bhaskar Bandikatla FRCA FFPMRCA.
The IBAP Way uses a structured, layered diagnostic approach: a detailed clinical history and neurological examination, followed by targeted investigations including MRI cervical spine, X-rays (including dynamic flexion-extension views), CT scans, nerve conduction studies with EMG, and blood tests to exclude inflammatory and systemic causes. Crucially, diagnostic spinal analgesia (DSA) — targeted nerve blocks at specific levels — is used to precisely confirm the pain generator before any interventional treatment is offered. This prevents unnecessary procedures and ensures treatment is directed at the correct source.
Yes. Whiplash and road-accident-related cervical injuries — extremely common in Hyderabad due to potholes, sudden braking, and two-wheeler accidents — most commonly cause soft tissue injuries, disc injuries, and facet joint damage, all of which are amenable to interventional treatment. Early diagnosis and targeted intervention can prevent the transition from acute to chronic pain syndrome. Surgery is rarely required for whiplash injuries. If you have been in a road accident and have persistent neck pain, early specialist assessment at IBAP Clinics is strongly advised.
Founder & Interventional Pain Specialist — IBAP Clinics, Hyderabad
MBBS · DA · FRCA (London) · FFPMRCA (Pain Medicine, UK) · MBA (Hospital Management)
CCT (Anaesthesia & Pain Medicine, UK) · Advanced Pain Training (Cambridge University Hospitals)
DDSMed Sports Medicine (Chicago) · Fellowship in Neuromodulation & Advanced Pain (London)
Dr Vijay brings over 15 years of postgraduate training across the United Kingdom’s most prestigious institutions — including the Royal College of Anaesthetists, Cambridge University Hospitals, and a dedicated neuromodulation fellowship in London — to his practice in Hyderabad. He is one of very few clinicians in India trained to the level of FFPMRCA — the Faculty of Pain Medicine of the Royal College of Anaesthetists — the highest qualification in pain medicine available in the UK.
His specialist expertise spans the full spectrum of knee pain management: from precision PRP and BMAC injections to cooled radiofrequency genicular nerve ablation, intrathecal drug delivery, and spinal cord stimulation for refractory pain states. He manages cases ranging from the weekend cricketer’s torn meniscus to the elderly cardiac patient with end-stage OA who has been told there are no further options.
2nd Floor, 284/A, Road No. 12, above IDFC First Bank, near Omega hospitals, MLA Colony, Banjara Hills, Hyderabad, Telangana 500034.
4th Floor, Plot no. 200, beside South India Shopping Mall, opp. Fortune Heights, Madeenaguda, Hyderabad, Telangana 500049

Indo-British Advanced Pain Clinic © 2026. All Rights Reserved. Designed & Developed By Adroit
WhatsApp us