Helpline :
9807 55 6789
-
Call Us Now: 9807 55 6789Call Us Now: 9807 55 6789
Expert non-surgical management of all shoulder pain conditions — from frozen shoulder and rotator cuff tears to shoulder OA, impingement, and labral pathology.
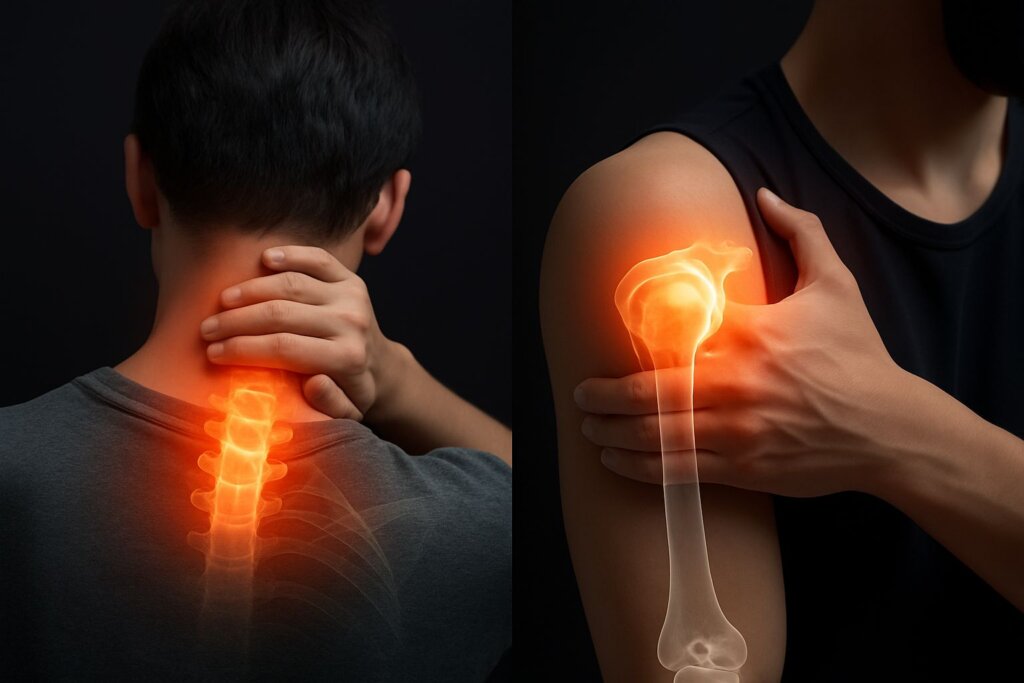
Shoulder pain is pain arising in or around the glenohumeral joint, acromioclavicular joint, surrounding tendons, bursae, or joint capsule — with or without radiation into the arm, neck, or hand. It is the third most common musculoskeletal complaint worldwide, after low back pain and neck pain, and a leading cause of functional disability in working-age adults in India.
Think of the shoulder as the most mobile joint in the human body — it trades the deep bony stability of the hip for extraordinary range of motion. The ball (humeral head) sits on the glenoid, a shallow cup roughly the size of a golf tee holding a golf ball. This freedom of movement comes at a price: the shoulder is inherently vulnerable to injury, degeneration, and inflammation.
| Structure | Key Role | When It Goes Wrong | |
|---|---|---|---|
| 🎯 | Glenohumeral Joint | Primary ball-and-socket articulation | Frozen shoulder, OA, instability, labral tears |
| 💪 | Rotator Cuff (SITS) | Dynamic humeral head centration | Tendinosis, partial & full-thickness tears |
| 🦴 | Subacromial Space | Cushions cuff under acromion | Impingement, bursitis, cuff compression |
| 💧 | Subacromial Bursa | Reduces tendon friction | Bursitis; calcific tendinitis deposit site |
| 🔵 | Glenoid Labrum | Deepens socket; biceps anchor | SLAP tears, Bankart lesions, instability |
| ➕ | AC Joint | Clavicle-scapula articulation | OA, sprains, Grade IV–VI dislocations |
| 🌐 | Joint Capsule | Encapsulates GH joint | Adhesive capsulitis (frozen shoulder) |
Shoulder pain is rarely a diagnosis in itself it is a symptom with many potential structural, metabolic, inflammatory, and referred causes. The following conditions are all part of the same shoulder pain pathology continuum. Most can be managed effectively without surgery when accurately diagnosed and appropriately treated.
Chronic degenerative thickening of the rotator cuff tendons — most commonly the supraspinatus — without active inflammation. A leading cause of shoulder pain in adults aged 30–55. Associated with repetitive overhead work and sports. Responds well to PRP therapy and structured physiotherapy.
→ /conditions/rotator-cuff-tendinosis
Partial or complete breach of one or more rotator cuff tendons. Over 90% involve the supraspinatus. Tears may be acute (traumatic) or chronic (degenerative). Not all tears require surgery — partial tears and many full-thickness tears in lower-demand individuals respond excellently to regenerative therapy.
→ /conditions/rotator-cuff-tearProgressive contraction and fibrosis of the glenohumeral joint capsule — causing severe pain followed by global loss of movement. Three stages: Freezing, Frozen, Thawing. Strongly associated with diabetes mellitus and thyroid disorders. The IBAP 5-stage hydrodilatation protocol achieves excellent results without surgery.
Degenerative loss of articular cartilage in the shoulder ball-and-socket joint. Less common than hip or knee OA but profoundly disabling when severe. Causes include age, prior fractures, massive rotator cuff tears (cuff arthropathy), and inflammatory arthritis. Managed with PRP, BMAC, and Cooled RFA.
Acromioclavicular joint OA causes focal pain at the top of the shoulder, worsened by cross-body movements and bench pressing. AC joint sprains (Grade I–VI) result from direct falls. Grades I–III managed non-surgically. Targeted AC joint injection (steroid or PRP) is highly effective for OA-related pain.
→ /conditions/ac-jointMechanical compression of the subacromial bursa and rotator cuff between the humeral head and the acromion. The most common cause of shoulder pain in overhead workers and athletes. Presents with a painful arc of motion (60–120° abduction). Highly responsive to subacromial injection and physiotherapy.
→ /conditions/shoulder-impingementRheumatoid arthritis affects the shoulder in up to 65% of RA patients. Distinguished from OA by morning stiffness >45 minutes, elevated CRP/ESR/RF, and systemic features. Guided steroid and PRP injections complement — but do not replace — DMARD/biologic therapy from a rheumatologist.
Tear of the superior glenoid labrum at the biceps anchor. Common in overhead athletes — cricketers, volleyball players, swimmers, weightlifters. Mechanism: repetitive traction or fall on outstretched arm. Symptoms: deep pain, clicking, weakness overhead. MR arthrogram is diagnostic. PRP first; arthroscopic repair after 6 months of failed conservative care.
Anteroinferior labral tear from anterior shoulder dislocation. Common in contact athletes aged 15–35. Each subsequent dislocation increases re-injury risk. Bony Bankart (glenoid rim avulsion) is a more serious variant. First-time dislocators in lower-demand individuals: physiotherapy. Recurrent instability (>2 events): arthroscopic Bankart repair.
→ /conditions/bankart-lesionHydroxyapatite crystal deposits within the rotator cuff trigger an acute, intensely painful inflammatory reaction — one of the most acutely painful shoulder conditions encountered clinically, often waking patients at night. Diagnosed on X-ray and ultrasound. Highly responsive to ultrasound-guided barbotage (needle aspiration and lavage).
Long head of biceps tendon (LHBT) causes anterior shoulder pain with bicipital groove tenderness. Positive Speed’s and Yergason’s tests. LHBT rupture causes a Popeye deformity — cosmetically apparent but functionally well-tolerated in older adults. Managed with ultrasound-guided bicipital sheath injection (steroid or PRP) and physiotherapy.
Cervical disc disease at C4/5 or C5/6 frequently refers pain to the shoulder — mimicking intrinsic shoulder pathology. Differentiated by: shoulder pain reproduced by neck compression (Spurling’s test), associated neurological symptoms, and a normal shoulder examination. Other referred causes: diaphragmatic irritation (liver, subphrenic abscess), Pancoast tumour (lung apex), and cardiac ischaemia (left shoulder). A complete systemic review is mandatory in all atypical shoulder pain presentations. Treating the shoulder without addressing the true source yields consistently disappointing results.
→ /conditions/referred-shoulder-pain🎯 Aching pain at the top or outer shoulder : Persistent deep soreness at the deltoid insertion or supraspinatus footprint — typically tendinosis or impingement
🎯 Painful arc of motion (60–120° of abduction):Pain specifically in a mid-range arc of elevation — the hallmark of subacromial impingement and early rotator cuff tear
🎯 Global loss of movement in all planes: Equally restricted active and passive motion in all directions — the cardinal sign of frozen shoulder (adhesive capsulitis)
🎯 Night pain and difficulty sleeping on the shoulder: Pain disrupting sleep or worsening when lying on the affected side — common in all cuff pathologies and frozen shoulder
🎯 Weakness with overhead reaching or lifting: Difficulty elevating the arm against resistance — indicates significant rotator cuff tear, impingement, or nerve involvement
🎯 Clicking, clunking, or catching sensation: Mechanical sounds or sensations during shoulder movement — labral tear (SLAP, Bankart), loose body, or AC joint pathology
🎯 Sharp pain reaching behind the back: Internal rotation restriction — classic of frozen shoulder, subscapularis pathology, and glenohumeral OA
🎯 Arm pain, numbness, or tingling to the hand: Neurological symptoms — suggests cervical radiculopathy, thoracic outlet syndrome, or suprascapular nerve entrapment rather than primary shoulder pathology
Warning Signs — Seek Urgent Medical Attention

At IBAP Clinics, we treat the cause — not just the symptom. Accurate identification of the pain generator is the prerequisite for any effective treatment. Our diagnostic process mirrors UK interventional pain medicine standards.

Thorough consultation exploring onset, character, radiation, aggravating and relieving factors, and functional impact. Validated tools (VAS, DASH, ASES shoulder score). Metabolic screening (diabetes, thyroid) for all frozen shoulder presentations.

Range of motion (active and passive), rotator cuff strength testing, impingement provocation tests (Hawkins-Kennedy, Neer), instability tests, labral tests (O'Brien's, Biceps Load), and cervical spine screening (Spurling's). Distinguishes intrinsic shoulder pathology from referred cervicogenic pain.

Real-time, dynamic assessment of the rotator cuff, biceps tendon, subacromial bursa, and AC joint. Unlike MRI, ultrasound allows the shoulder to be moved during scanning to identify impingement and assess cuff integrity dynamically. The gold standard for guiding shoulder injections.

Imaging interpreted within clinical context — degenerative changes are present in over 50% of asymptomatic adults over 50. MRI is the gold standard for soft tissue, labrum, and full-thickness cuff assessment. MR arthrogram for labral pathology (SLAP, Bankart). X-ray for bony morphology, calcific deposits, and joint space.

Targeted diagnostic injections — subacromial local anaesthetic blocks, glenohumeral injections, AC joint blocks, and selective suprascapular nerve blocks — can confirm the structural pain source before committing to definitive treatment. A positive diagnostic block confirms both the diagnosis and the treatment target.

A tailored treatment pathway designed from all of the above — from targeted guided injections and regenerative therapies to hydrodilatation for frozen shoulder, Cooled RFA for refractory arthritic pain, and structured physiotherapy rehabilitation. Surgery recommended only when non-surgical options have been comprehensively exhausted.
Our treatment philosophy is precision over generalisation. We match the intervention to the structural diagnosis — delivered under ultrasound or fluoroscopic guidance — to maximise efficacy and minimise risk. All procedures are performed to UK interventional pain medicine standards.
FIRST-LINE INTERVENTION
FROZEN SHOULDER · HYDRAULIC DISTENSION
SUPRASCAPULAR NERVE · TARGETED BLOCK
REGENERATIVE · BLOOD-DERIVED
REGENERATIVE · BONE MARROW
Bone marrow aspirate from the patient’s iliac crest is concentrated to yield mesenchymal stem cells (MSCs), platelets, cytokines, and growth factors. MSCs can differentiate into cartilage, tendon, and bone — offering genuine structural repair potential beyond growth factor stimulation alone. Deployed at IBAP Clinics for moderate-to-severe glenohumeral OA, large partial-thickness RCTs, cuff arthropathy, and refractory tendinosis with significant MRI changes. Same-day procedure under fluoroscopic guidance.
ADVANCED · COOLED RF
NEUROMODULATORY RF
PRF delivers radiofrequency energy in short bursts, maintaining tissue temperature below 42°C — modulating rather than destroying nerve conduction. Suitable for the suprascapular nerve where thermal ablation carries motor risk. Indicated for post-operative shoulder pain, frozen shoulder neuralgia, and younger patients where reversible neuromodulation is preferred.
ESSENTIAL BASELINE CARE
Physiotherapy is the backbone of all shoulder pain management — no intervention, however sophisticated, delivers lasting results without concurrent musculotendinous rehabilitation. Diagnosis-driven approach:
For the majority of shoulder conditions, surgery is not the first step. The IBAP Clinics principle: exhaust all evidence-based non-surgical options, in a structured and time-defined manner, before considering surgical referral. Surgery carries real risks — the decision must always weigh expected benefit against complication profile.
Acute, traumatic full-thickness RCT in active patient (<60 yrs) — repair within 3–6 months
Bankart lesion with recurrent anterior instability (>2 dislocations) in an athlete
SLAP Type II–IV with failed 6 months of structured non-surgical treatment in overhead athlete
End-stage glenohumeral OA with severe daily functional restriction unresponsive to all non-surgical care
Massive irreparable RCT causing pseudo-paralysis in a surgical candidate
Septic arthritis — surgical washout is urgent and non-negotiable
Partial-thickness RCT — excellent response to PRP or BMAC + physiotherapy
Frozen shoulder (any stage) — hydrodilatation + post-procedure physiotherapy first
Subacromial impingement without structural tear — injection + physiotherapy highly effective
Mild–moderate glenohumeral OA — Cooled RFA, BMAC, or PRP provides substantial durable relief
Full-thickness RCT in patients over 65 with low functional demand — non-surgical outcomes comparable
Calcific tendinitis — ultrasound-guided barbotage is curative in most cases
Key principle: when surgery is decided upon, it should be performed promptly by an experienced shoulder surgeon. Delay beyond the surgical window — particularly for acute full-thickness RCTs — leads to tendon retraction, fatty infiltration, and irreparability. The pain specialist’s role is not to delay surgery indefinitely, but to ensure it is undertaken for the right diagnosis, at the right time, in the right patient.
These questions reflect the most common searches by patients with shoulder pain. All answers authored by Dr Vijay Bhaskar Bandikatla, Interventional Pain Specialist, IBAP Clinics.
The most common causes are rotator cuff tendinopathy, subacromial impingement syndrome, and frozen shoulder (adhesive capsulitis). Frozen shoulder has particularly high prevalence in the Indian population, driven by elevated rates of Type 2 diabetes and thyroid disorders. In South India, occupational overuse (IT professionals, manual workers) and sports injuries (cricket, gym) contribute significantly. At IBAP Clinics, frozen shoulder and rotator cuff conditions together account for the majority of shoulder pain presentations.
Yes — the vast majority of frozen shoulder cases can and should be treated without surgery. The IBAP Clinics 5-stage protocol (targeted corticosteroid injection → fluoroscopy-guided hydrodilatation → structured physiotherapy → progressive strengthening) achieves excellent outcomes in 85–90% of patients. Arthroscopic capsular release is reserved for the small minority who fail comprehensive non-surgical management after 12 months.
No. Many full-thickness rotator cuff tears — particularly in adults over 60 with moderate functional demands — can be managed effectively without surgery, achieving outcomes comparable to operative repair. Partial-thickness tears respond very well to PRP or BMAC injections combined with structured physiotherapy. Surgery is primarily indicated for acute, traumatic full-thickness tears in young, active individuals (under 60 years), or for massive tears causing pseudo-paralysis.
Both are regenerative therapies from the patient’s own body. PRP concentrates growth factors from a blood sample — ideal for tendinopathy, partial tears, and mild OA. BMAC goes further, concentrating mesenchymal stem cells from bone marrow — capable of differentiating into cartilage, tendon, and bone for genuine structural regeneration. BMAC is preferred for more advanced OA and larger partial tears where structural rebuilding is needed. Both performed under image guidance as same-day procedures at IBAP Clinics.
Cooled Radiofrequency Ablation ablates the sensory articular nerve branches supplying the shoulder joint — switching off the pain signal at source without affecting motor function. Particularly effective for shoulder OA and cuff arthropathy. Pain relief typically lasts 9–18 months; the procedure can be safely repeated as nerves regenerate. An excellent option for patients unsuitable for or wishing to delay shoulder replacement surgery
A SLAP tear (Superior Labrum Anterior to Posterior) is a tear of the superior glenoid labrum at the long head of biceps attachment. Most common in overhead athletes — cricketers, volleyball players, swimmers, weightlifters — from repetitive traction or a fall on an outstretched arm. Symptoms: deep shoulder pain, clicking, weakness with overhead activities. MR arthrogram is diagnostic. PRP first; arthroscopic repair for Type II–IV tears after 6 months of failed non-surgical care.
If your shoulder pain persists beyond 6 weeks, is worsening, is accompanied by arm weakness or numbness, severely restricts daily activities, or is not responding to physiotherapy and anti-inflammatory medication. Early specialist assessment prevents unnecessary chronicity. Contact IBAP Clinics on +91 98075 56789 to book at Banjara Hills or Madeenaguda, Hyderabad.
At IBAP Clinics (+91 98075 56789), Dr Vijay Bhaskar offers: ultrasound-guided corticosteroid injections (subacromial, glenohumeral, AC joint), suprascapular nerve blocks, hydrodilatation for frozen shoulder, PRP therapy, BMAC regenerative injection, Cooled RFA, pulsed radiofrequency of the suprascapular nerve, and structured post-procedural physiotherapy rehabilitation — all to UK interventional pain medicine standards.
2nd Floor, 284/A, Road No. 12, above IDFC First Bank, near Omega hospitals, MLA Colony, Banjara Hills, Hyderabad, Telangana 500034.
4th Floor, Plot no. 200, beside South India Shopping Mall, opp. Fortune Heights, Madeenaguda, Hyderabad, Telangana 500049

Indo-British Advanced Pain Clinic © 2026. All Rights Reserved. Designed & Developed By Adroit
WhatsApp us